The Ultimate Guide to Medical Billing for Mental Health in the USA: Strategies to Maximize Revenue and Reduce Claim Denials
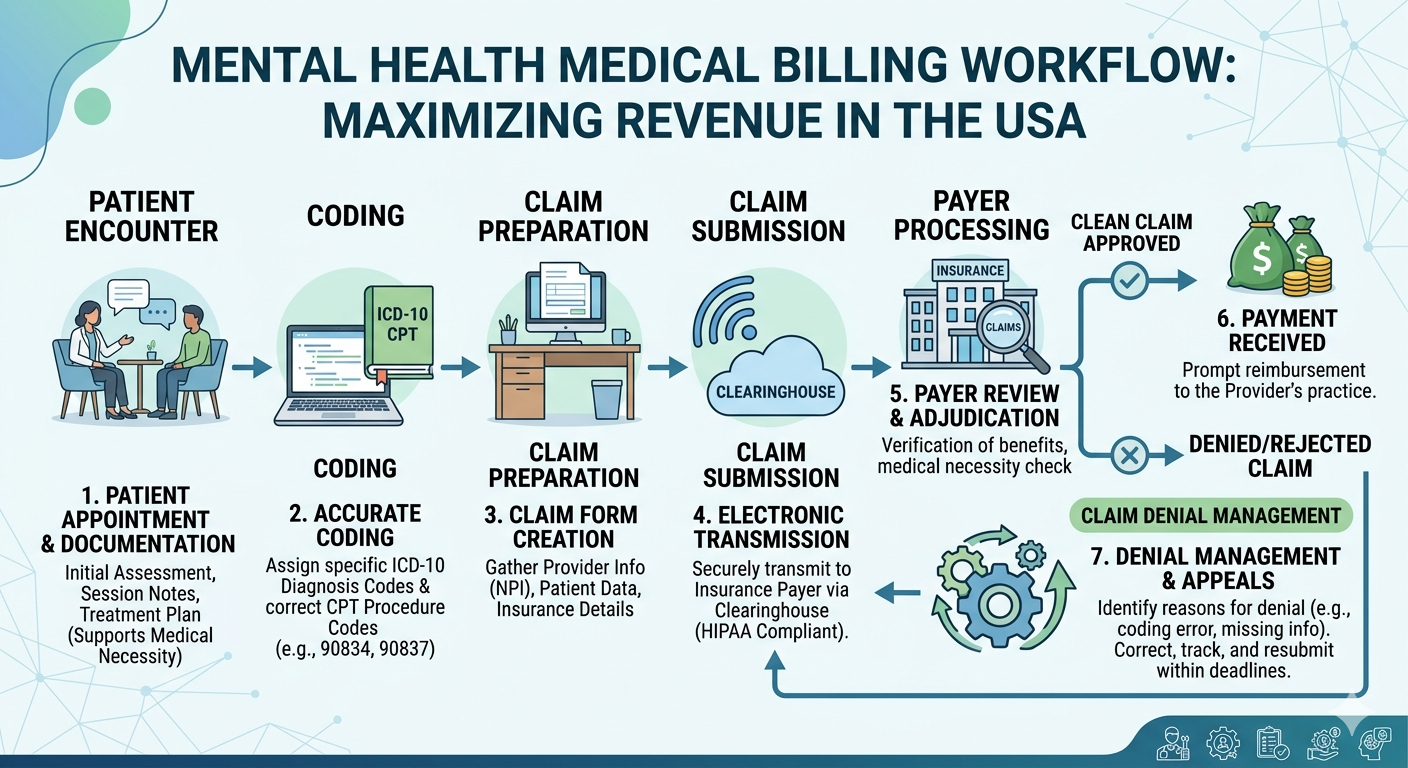
Mental health practices across the USA are growing rapidly, but with that growth comes a complex challenge—managing billing efficiently. Unlike general healthcare billing, medical billing for mental health involves unique coding structures, therapy session variations, insurance nuances, and strict compliance requirements.
Whether you're a solo therapist, a multi-provider clinic, or expanding your behavioral health practice, understanding how billing works can directly impact your revenue, compliance, and patient satisfaction. This guide breaks down everything you need to know, with practical insights and strategies that actually work in real-world scenarios.
Why Medical Billing for Mental Health Is More Complex Than You Think
Mental health billing isn’t just about submitting claims—it’s about accuracy, timing, and understanding payer expectations. Even a minor mistake can lead to claim denials or delayed reimbursements.
Here’s what makes it challenging:
- Session-based billing instead of procedure-heavy models
- Frequent use of time-based CPT codes
- Strict documentation requirements
- Variability in payer rules for therapy coverage
- Pre-authorizations for certain treatments
For example, a therapist conducting a 60-minute psychotherapy session must ensure that the documentation aligns perfectly with the CPT code billed. If not, insurers may reject the claim.
Understanding Mental Health Insurance Billing Services
Many providers rely on mental health insurance billing services to streamline operations. These services specialize in handling behavioral health claims, ensuring compliance with insurance guidelines, and reducing administrative burdens.
A professional billing partner can help with:
- Insurance verification and eligibility checks
- Accurate coding and claim submission
- Denial management and appeals
- Payment posting and reporting
For growing practices, this support can mean the difference between steady cash flow and constant financial stress.
The Role of a Mental Health Billing Specialist
A mental health billing specialist is trained specifically in behavioral health coding and reimbursement processes. Their expertise ensures that claims are submitted correctly the first time.
Key responsibilities include:
- Assigning accurate CPT and ICD-10 codes
- Ensuring documentation meets payer requirements
- Monitoring claim status and follow-ups
- Handling denied or rejected claims
In smaller practices, hiring a dedicated specialist might not be feasible—which is why many providers choose to outsource.
Why Practices Choose to Outsource Mental Health Billing Services
Outsourcing has become a popular option for mental health providers across the USA. When you outsource mental health billing services, you gain access to a team of experts without the cost of in-house staff.
Benefits of outsourcing:
- Reduced administrative workload
- Faster claim processing
- Improved revenue collection
- Access to experienced billing professionals
- Compliance with changing regulations
For instance, a mid-sized therapy clinic in Texas reported a 25% increase in collections within three months after switching to outsourced mental health billing.
Choosing the Best Mental Health Billing Agency
Not all billing providers are created equal. Selecting the best mental health billing agency requires careful evaluation.
What to look for:
- Experience in behavioral health billing
- Transparent pricing structure
- Strong reporting and analytics
- HIPAA compliance
- Proven track record of reducing denials
A reliable mental health billing services agency will act as an extension of your practice—not just a vendor.
Key Components of Mental Health Medical Billing Services
Comprehensive mental health medical billing services go beyond claim submission. They cover the entire billing lifecycle.
Core services include:
1. Insurance Verification
Ensures patients are eligible for services before treatment begins.
2. Accurate Coding
Using proper CPT and ICD codes is critical for reimbursement.
3. Claim Submission
Clean claims reduce rejection rates and speed up payments.
4. Denial Management
Identifying and correcting issues quickly improves revenue.
5. Payment Posting
Keeps financial records accurate and up-to-date.
A well-rounded mental health medical billing solution integrates all these components seamlessly.
Billing Services for Mental Health Therapists: What Matters Most
For therapists, time is best spent with patients—not on paperwork. That’s why billing services for mental health therapists focus on simplicity and efficiency.
Important considerations:
- Ease of communication with billing team
- Real-time access to reports
- Transparency in claim status
- Support for multiple therapy modalities
Whether you're offering individual therapy, group sessions, or telehealth, your billing system should adapt accordingly.
The Value of a Mental Health Billing and Coding Company
A specialized mental health billing and coding company ensures that both billing and coding processes are aligned. Errors often occur when these two functions are disconnected.
Why integration matters:
- Reduces coding errors
- Improves claim acceptance rates
- Ensures compliance with payer guidelines
This is where medical coding services and medical billing and coding services play a crucial role in maintaining accuracy and consistency.
Mental Health Medical Billing Services Outsourcing: A Scalable Approach
As practices grow, managing billing internally becomes harder. Mental health medical billing services outsourcing offers scalability without increasing overhead costs.
Ideal for:
- Multi-location practices
- Expanding therapy clinics
- Telehealth providers
With outsourced mental health billing, practices can focus on patient care while experts handle the financial side.
How Top Outsource Mental Health Billing Companies Improve Revenue
A top outsource mental health billing company doesn’t just process claims—they optimize revenue.
Strategies they use:
- Identifying underpaid claims
- Reducing claim turnaround time
- Monitoring payer trends
- Implementing best practices in documentation
These improvements directly impact your bottom line.
Common Challenges Faced by Mental Health Billing Companies
Even experienced mental health billing companies face challenges such as:
- Frequent policy changes by insurers
- Complex authorization requirements
- Coding updates
- Patient billing disputes
However, a strong billing partner will proactively address these issues and keep your practice running smoothly.
Billing Services for Mental Health Providers: A Holistic Approach
Effective billing services for mental health providers combine technology, expertise, and strategy.
A holistic billing system includes:
- Automated workflows
- Data-driven insights
- Integration with EHR systems
- Continuous performance monitoring
When all these elements work together, practices experience fewer errors and better financial outcomes.
The Importance of Revenue Cycle Management in Mental Health
A strong billing system is part of a larger process known as revenue cycle management services. This includes everything from patient registration to final payment.
Key stages:
- Patient scheduling and registration
- Insurance verification
- Coding and charge entry
- Claim submission
- Payment posting
- Denial management
Efficient revenue cycle management ensures consistent cash flow and long-term sustainability.
Why Credentialing Services Are Critical
Before you can bill insurance companies, you must be properly credentialed. Credentialing services ensure that providers are authorized to deliver care and receive reimbursements.
Without proper credentialing:
- Claims may be denied
- Payments can be delayed
- Compliance risks increase
For new practices, this step is often overlooked—but it’s essential for success.
Real-World Example: Improving Billing Efficiency
A behavioral health clinic in California struggled with delayed payments and high denial rates. After partnering with a specialized mental health billing agency, they:
- Reduced denials by 40%
- Increased monthly revenue by 30%
- Improved patient billing transparency
This highlights the impact of choosing the right billing partner.
Final Thoughts: Building a Strong Financial Foundation
Navigating medical billing for mental health doesn’t have to be overwhelming. With the right systems, expertise, and support, practices can achieve consistent revenue growth while focusing on patient care.
Partnering with experienced providers like 247 medical billing services can make a meaningful difference. Their approach combines medical billing services, medical coding services, and medical billing and coding services with comprehensive revenue cycle management services and reliable credentialing services—all working together to support long-term success without disrupting your clinical workflow.
FAQs
1. What is medical billing for mental health?
Medical billing for mental health involves submitting and managing insurance claims for therapy and behavioral health services, ensuring providers are reimbursed accurately.
2. Why should I outsource mental health billing services?
Outsourcing reduces administrative workload, improves claim accuracy, and increases revenue by leveraging experienced billing professionals.
3. How do mental health billing specialists help?
They ensure accurate coding, manage claims, handle denials, and maintain compliance with insurance requirements.
4. What are the benefits of mental health medical billing services outsourcing?
It offers scalability, cost savings, faster reimbursements, and access to expert billing teams.
5. What should I look for in a mental health billing company?
Look for experience, transparency, compliance, strong reporting systems, and a proven track record.
6. How do revenue cycle management services improve practice performance?
They streamline the entire billing process—from patient intake to final payment—ensuring consistent cash flow and reduced errors.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Jocuri
- Gardening
- Health
- Home
- Literature
- Music
- Networking
- Alte
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness


