Why Outsourced Billing for Mental Health in USA Is Transforming Practice Profitability in 2026
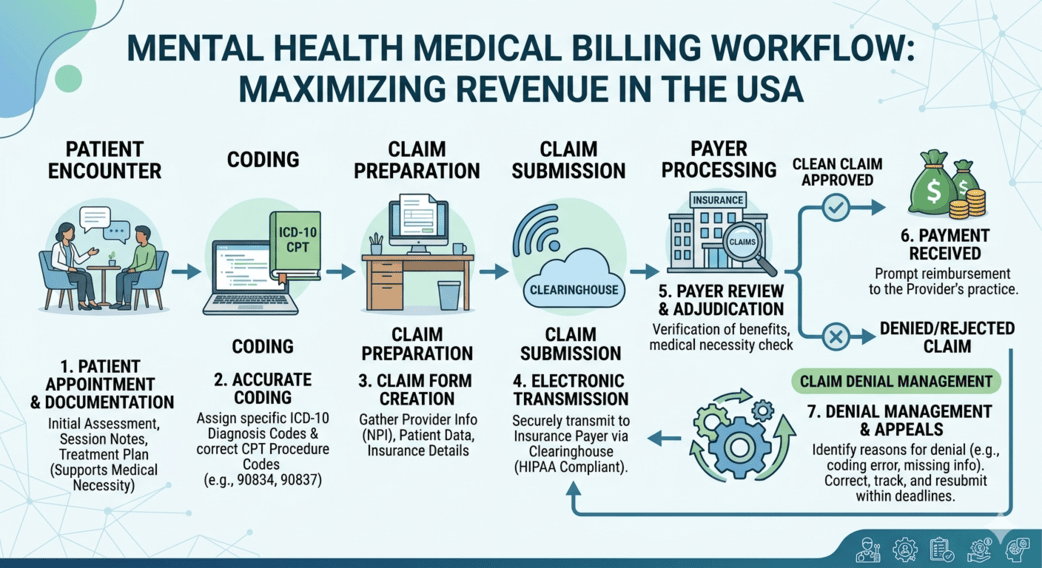
Mental health practices across the USA are growing rapidly—but so are administrative challenges. From evolving payer rules to complex documentation requirements, managing billing for mental health providers has become a time-consuming burden. Many clinics, therapists, and behavioral health groups are now turning to outsourced billing for mental health as a smarter, more sustainable solution.
This shift isn’t just about reducing workload—it’s about improving accuracy, accelerating reimbursements, and building a financially stable practice. Let’s explore how outsourcing is reshaping billing for mental health services and why it’s becoming essential in today’s healthcare landscape.
The Growing Complexity of Mental Health Billing
Mental health billing is not as straightforward as general medical billing. It involves:
- Time-based CPT codes
- Frequent changes in payer policies
- Strict documentation requirements
- Pre-authorizations and eligibility checks
- Compliance with Medicare and private insurers
For providers handling billing mental health internally, even small errors can lead to claim denials or delayed payments.
Example:
A therapist submitting claims for extended sessions without proper time documentation may face repeated denials. Over time, this impacts cash flow and operational efficiency.
That’s where mental health billing solutions come into play—especially outsourced ones.
What Is Outsourced Billing for Mental Health?
Outsourcing mental health billing means partnering with a specialized team that handles:
- Claim submission and tracking
- Insurance verification
- Payment posting
- Denial management
- Compliance monitoring
These experts focus exclusively on medical billing for mental health, ensuring higher accuracy and faster reimbursements.
Why Mental Health Providers Are Choosing Outsourcing
1. Improved Revenue Cycle Performance
Outsourcing helps streamline your entire billing workflow. With professional revenue cycle management services, practices can:
- Reduce claim denials
- Speed up reimbursements
- Improve cash flow
Instead of chasing unpaid claims, providers can focus on patient care.
2. Access to Specialized Expertise
Billing for mental health therapists requires deep knowledge of:
- CPT and ICD-10 codes
- Behavioral health payer policies
- Telehealth billing regulations
Outsourced teams offering medical coding services ensure every claim is coded accurately, minimizing errors.
3. Cost Efficiency Without Compromise
Hiring and training an in-house billing team is expensive. Outsourcing offers access to:
- Experienced professionals
- Advanced billing software
- Scalable solutions
Many practices even find a cheap outsource mental health billing company that delivers high-quality services at a fraction of the cost.
4. Better Compliance and Reduced Risk
With constant regulatory updates, compliance is a major concern. Outsourced providers offering mental health billing and credentialing services help ensure:
- HIPAA compliance
- Accurate documentation
- Proper payer credentialing
This reduces audit risks and financial penalties.
Key Services Included in Mental Health Billing Outsourcing
A reliable partner typically provides comprehensive behavioral and mental health billing services, including:
Eligibility Verification
Ensures patient coverage before services are delivered.
Coding and Billing
Accurate coding and billing for mental health services using updated guidelines.
Claims Submission
Clean claims submission to reduce rejections.
Denial Management
Quick identification and correction of denied claims.
Payment Posting
Transparent tracking of payments and adjustments.
Reporting & Analytics
Insights into financial performance and billing trends.
The Role of Medicare in Mental Health Billing
Billing Medicare for mental health services requires strict adherence to guidelines. Errors in:
- Session duration
- Documentation
- Provider eligibility
can result in rejected claims.
Outsourced experts understand Medicare policies and ensure compliance, helping providers maximize reimbursements.
Challenges of In-House Billing for Mental Health Clinics
While some clinics manage billing internally, they often face:
- Staff burnout
- Frequent coding errors
- Delayed reimbursements
- Limited scalability
For growing practices, relying solely on in-house teams can slow down operations.
How to Choose the Best Outsource Mental Health Billing and Coding Services
Not all providers are the same. When selecting a partner, consider:
Experience in Mental Health Billing
Choose a team specializing in mental health medical billing, not general billing.
Technology & Tools
Look for advanced billing systems with real-time tracking.
Transparency
Clear reporting and communication are essential.
Scalability
Ensure they can grow with your practice.
Compliance Standards
They should follow HIPAA and payer-specific regulations.
Real-World Impact: A Practice Transformation Story
A mid-sized behavioral health clinic in Texas struggled with delayed payments and high denial rates. After switching to outsourced billing services for mental health clinics, they experienced:
- 35% reduction in claim denials
- 25% faster reimbursements
- Significant administrative cost savings
This allowed their team to focus more on patient care rather than paperwork.
The Connection Between Billing and Patient Care
Efficient billing doesn’t just impact revenue—it improves patient experience.
When billing processes are smooth:
- Patients receive accurate invoices
- Insurance claims are processed faster
- Administrative delays are minimized
This builds trust and enhances overall satisfaction.
Integrating Credentialing with Billing
Credentialing is often overlooked but plays a critical role in reimbursement.
Outsourced providers offering credentialing services ensure:
- Providers are enrolled with insurance networks
- Claims are not rejected due to credentialing issues
- Faster onboarding for new practitioners
Combining credentialing with billing creates a seamless workflow.
The Future of Mental Health Billing in the USA
The demand for mental health services continues to rise, and so does the need for efficient billing systems. Trends shaping the future include:
- AI-driven claim processing
- Automated eligibility verification
- Telehealth billing expansion
- Value-based care models
Practices that adopt outsourcing mental health billing early will have a competitive advantage.
A Practical Approach to Transitioning to Outsourced Billing
Switching to outsourcing doesn’t have to be overwhelming. A smooth transition involves:
- Evaluating current billing performance
- Identifying pain points
- Choosing the right billing partner
- Gradual data migration
- Continuous performance monitoring
With the right approach, practices can transition without disrupting operations.
Why Partnering with the Right Billing Provider Matters
A trusted partner doesn’t just handle claims—they become an extension of your practice.
Companies like 247 medical billing services offer integrated support that includes:
- Medical billing services tailored to mental health practices
- Medical coding services ensuring accurate claim submission
- Medical billing and coding services that align with payer requirements
- Revenue cycle management services for end-to-end financial optimization
- Credentialing services to ensure provider eligibility and faster reimbursements
This holistic approach helps practices achieve long-term financial stability while maintaining compliance.
Conclusion
Outsourced billing for mental health is no longer just an option—it’s becoming a necessity for modern practices in the USA. With increasing administrative demands and complex payer requirements, outsourcing offers a practical way to improve efficiency, reduce errors, and enhance revenue.
By leveraging expert mental health billing services, providers can focus on what truly matters: delivering quality care to their patients.
FAQs
1. What is outsourced billing for mental health?
Outsourced billing for mental health involves hiring a specialized company to manage billing tasks such as coding, claims submission, and payment tracking for mental health providers.
2. Is outsourcing mental health billing cost-effective?
Yes, outsourcing reduces staffing costs, minimizes errors, and improves reimbursement rates, making it a cost-effective solution for most practices.
3. How does outsourcing improve revenue cycle management?
It streamlines processes like claim submission, denial management, and payment posting, leading to faster reimbursements and improved cash flow.
4. Can outsourcing help with Medicare billing for mental health services?
Absolutely. Experienced billing teams understand Medicare guidelines and ensure accurate claim submission to reduce denials.
5. What services are included in mental health billing outsourcing?
Services typically include insurance verification, coding, claims submission, denial management, reporting, and credentialing.
6. How do I choose the best mental health billing company?
Look for experience in mental health billing, strong compliance practices, transparent reporting, and scalable solutions tailored to your practice.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Oyunlar
- Gardening
- Health
- Anasayfa
- Literature
- Music
- Networking
- Diğer
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness


