The Future of Mental Health Medical Billing Solution in the USA: Smarter, Faster, and Revenue-Driven
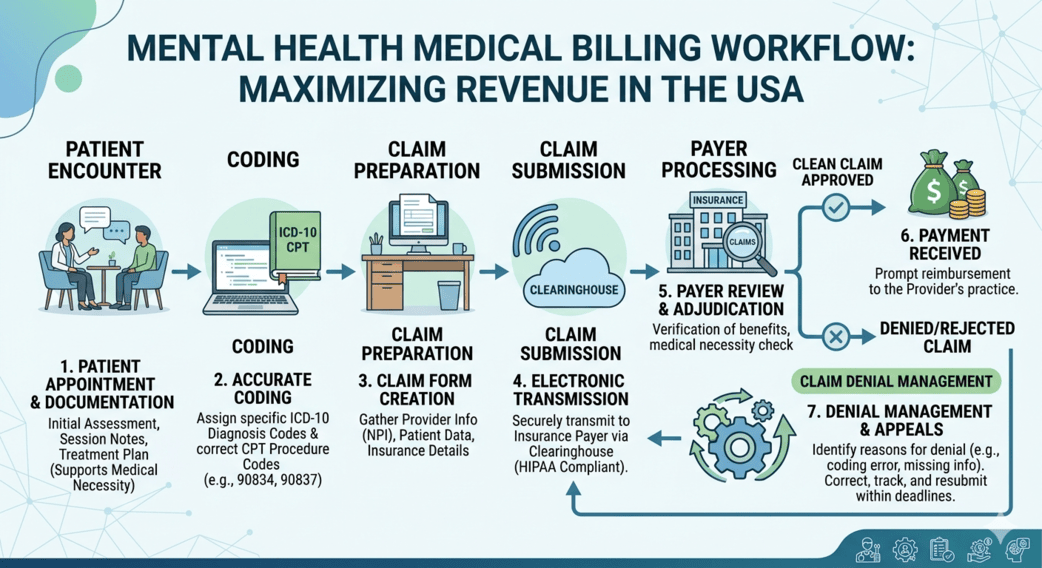
Mental health practices across the USA are evolving rapidly—but billing systems often lag behind. From complex insurance rules to frequent claim denials, providers face mounting administrative burdens that directly impact revenue and patient care. This is where a mental health medical billing solution becomes not just helpful, but essential.
Whether you're a solo therapist, a group practice, or a behavioral health clinic, understanding how modern billing solutions work can transform your financial health. Let’s explore how.
Why Mental Health Billing Is More Complex Than Ever
Mental health billing is not the same as general medical billing. It comes with its own unique challenges:
- Constantly changing payer policies
- Session-based billing structures
- Pre-authorization requirements
- Strict documentation standards
- High denial rates
Unlike other specialties, even minor coding errors can delay reimbursements for weeks. That’s why many providers now rely on mental health insurance billing services to stay compliant and efficient.
What Is a Mental Health Medical Billing Solution?
A mental health medical billing solution is a specialized system or service designed to handle the unique billing needs of behavioral health providers. It includes:
- Claims submission and tracking
- Insurance verification
- Coding accuracy checks
- Denial management
- Payment posting
In most cases, these solutions are offered by a mental health billing services agency or integrated software platforms.
The Role of a Mental Health Billing Specialist
A mental health billing specialist understands the nuances of psychotherapy codes, telehealth billing, and insurance guidelines. Their expertise ensures:
- Accurate CPT and ICD coding
- Reduced claim rejections
- Faster reimbursements
- Compliance with regulations
Without a specialist, practices often face revenue leakage due to overlooked details.
Benefits of Outsourcing Mental Health Billing Services
Many providers now prefer to outsource mental health billing services rather than managing everything in-house. Here’s why:
1. Reduced Administrative Burden
Outsourcing frees up your staff, allowing them to focus on patient care rather than paperwork.
2. Higher Claim Acceptance Rates
A professional mental health billing company ensures clean claims submission, minimizing denials.
3. Cost Efficiency
Hiring, training, and maintaining an in-house team can be expensive. Outsourced mental health billing offers a scalable solution.
4. Access to Experts
Working with a mental health billing consultant or agency gives you access to experienced professionals.
Choosing the Best Mental Health Billing Agency
Not all billing partners are created equal. When selecting the best mental health billing agency, consider:
- Experience in behavioral health
- Transparency in reporting
- Compliance with HIPAA regulations
- Technology integration capabilities
- Proven track record
A reliable mental health billing provider should act as a strategic partner—not just a service vendor.
Key Services Included in Mental Health Billing Solutions
A comprehensive mental health medical billing services outsourcing package typically includes:
Insurance Verification
Ensures patient eligibility before services are rendered.
Coding and Documentation
Accurate coding using up-to-date guidelines is critical. This is where medical coding services play a vital role.
Claims Submission
Timely and accurate claim filing increases approval rates.
Denial Management
Quick identification and correction of denied claims.
Accounts Receivable Follow-Up
Ensures outstanding payments are collected efficiently.
How Technology Is Changing Mental Health Billing
Modern mental health billing companies are leveraging technology to improve efficiency:
- AI-driven claim scrubbing
- Automated eligibility checks
- Real-time reporting dashboards
- Telehealth billing optimization
These innovations reduce manual errors and improve revenue cycles.
Real-World Scenario: A Growing Therapy Practice
Consider a mid-sized therapy clinic struggling with delayed payments. Their in-house billing team was overwhelmed, leading to:
- 30% claim denial rate
- Delayed reimbursements
- Staff burnout
After partnering with a top outsource mental health billing company, they experienced:
- 95% clean claim rate
- Faster payment cycles
- Improved cash flow
This is the tangible impact of a well-implemented mental health billing and coding company.
The Importance of Revenue Cycle Management in Mental Health
Billing is just one part of the bigger picture. Effective revenue cycle management services ensure that every stage—from patient intake to final payment—is optimized.
Key components include:
- Patient scheduling and verification
- Charge capture
- Claims processing
- Payment posting
- Reporting and analytics
When integrated with medical billing and coding services, RCM becomes a powerful tool for growth.
Why Credentialing Services Matter
Before billing can even begin, providers must be credentialed with insurance payers. Credentialing services ensure that:
- Providers are authorized to bill insurers
- Claims are not rejected due to enrollment issues
- Practice expansion is smooth and compliant
Without proper credentialing, even the best billing system can fail.
In-House vs. Outsourced Mental Health Billing
| Feature | In-House Billing | Outsourced Mental Health Billing |
|---|---|---|
| Cost | High | Cost-effective |
| Expertise | Limited | Specialized experts |
| Scalability | Low | High |
| Error Rate | Higher | Lower |
| Technology Access | Limited | Advanced tools |
For most practices, outsourced mental health billing offers a better return on investment.
Common Mistakes in Mental Health Billing
Avoid these pitfalls:
- Incorrect CPT codes
- Missing documentation
- Delayed claim submission
- Ignoring denied claims
- Lack of follow-up
Working with a mental health billing agency can help eliminate these issues.
How to Identify the Right Billing Partner
Look for a best outsource mental health billing and coding company that:
- Understands mental health workflows
- Offers transparent reporting
- Provides dedicated support
- Uses advanced billing software
- Aligns with your practice goals
The Future of Mental Health Billing in the USA
As mental health awareness grows, so does demand for efficient billing systems. The future will likely include:
- AI-powered automation
- Value-based reimbursement models
- Integrated EHR and billing systems
- Enhanced compliance tracking
Practices that adopt modern mental health medical billing solutions early will gain a competitive edge.
A Note on Choosing the Right Support System
Behind every successful billing operation is a strong support system. Providers often rely on integrated medical billing services, medical coding services, and comprehensive medical billing and coding services to maintain accuracy and compliance.
Additionally, revenue cycle management services and credentialing services play a crucial role in ensuring long-term financial stability.
Companies like 247 medical billing services have built their reputation by offering end-to-end solutions tailored for healthcare providers, including mental health practices—helping them navigate complex billing landscapes without disrupting patient care.
Conclusion
A well-structured mental health medical billing solution is no longer optional—it’s a necessity in today’s healthcare environment. From reducing administrative stress to improving cash flow, the right billing approach can transform your practice.
Whether you choose to manage billing in-house or partner with a mental health billing services agency, the goal remains the same: accuracy, efficiency, and sustainable growth.
FAQs
1. What is a mental health medical billing solution?
A mental health medical billing solution is a specialized service or system designed to handle billing, coding, and insurance claims for mental health providers.
2. Why should I outsource mental health billing services?
Outsourcing reduces administrative workload, improves claim accuracy, and ensures faster reimbursements.
3. How do mental health billing companies improve revenue?
They optimize claim submissions, reduce denials, and manage the entire revenue cycle efficiently.
4. What services are included in mental health billing?
Services include insurance verification, coding, claims submission, denial management, and payment posting.
5. How do I choose the best mental health billing agency?
Look for experience, transparency, compliance, and proven results in behavioral health billing.
6. What role does credentialing play in billing?
Credentialing ensures providers are authorized to bill insurance companies, preventing claim rejections.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Games
- Gardening
- Health
- Home
- Literature
- Music
- Networking
- Other
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness


