Mental Health Billing Columbus: Why Local Practices Are Turning to Specialized Billing Support
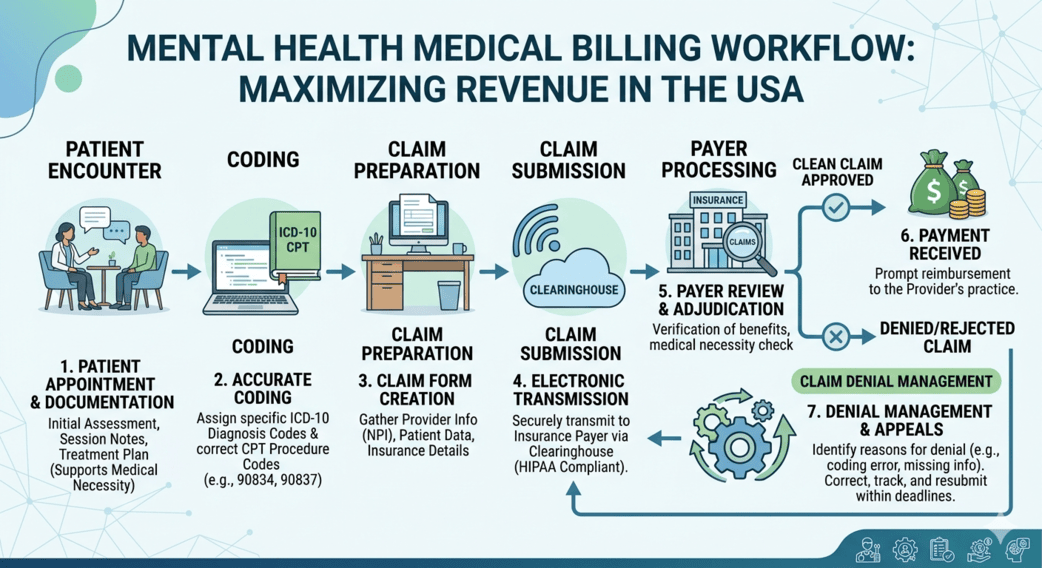
Running a mental health practice in Columbus today involves far more than patient care. Therapists, psychologists, psychiatrists, and behavioral health clinics are balancing increasing documentation requirements, insurance complexities, payer policy updates, and growing patient expectations—all while trying to maintain healthy cash flow.
For many providers, billing has quietly become one of the biggest operational burdens in the practice.
Claims that look accurate can still get denied. Small coding errors may delay reimbursements for weeks. Credentialing issues can interrupt payments entirely. And when administrative work starts consuming clinical time, patient experience often suffers too.
That’s why more behavioral health professionals are reevaluating how they manage their revenue cycle. The demand for specialized mental health billing Columbus providers has grown rapidly because practices want systems that actually understand behavioral healthcare—not just generic medical billing.
Mental health reimbursement comes with its own set of challenges, from time-based CPT coding and telehealth modifiers to authorization tracking and documentation audits. Practices that work with specialists in behavioral health billing often see fewer denials, faster payments, and better financial visibility.
The Billing Challenges Unique to Mental Health Practices
Behavioral healthcare billing is different from many other medical specialties. A family practice may bill straightforward office visits, but mental health claims often involve layered payer rules and stricter documentation expectations.
Consider a common scenario in Columbus: a therapist conducts a 60-minute psychotherapy session through telehealth for a patient covered by a commercial insurance plan. The claim may require:
- Correct psychotherapy CPT coding
- Telehealth modifiers
- Updated place-of-service indicators
- Prior authorization validation
- Timely documentation submission
- Compliance with payer-specific behavioral health policies
A single missing detail can delay reimbursement.
This is one reason many providers seek billing services for mental health therapists that specialize specifically in behavioral health workflows instead of general healthcare billing.
Common Obstacles Practices Face
Frequent Claim Denials
Mental health claims are denied for reasons that often appear minor on the surface:
- Incorrect session duration coding
- Missing modifiers
- Credentialing mismatches
- Authorization errors
- Incomplete progress notes
Repeated denials create cash flow instability and administrative overload.
Complex Insurance Verification
Behavioral health coverage varies significantly between plans. Even within the same insurer, benefits may differ for:
- Individual therapy
- Group therapy
- Family counseling
- Psychiatric evaluations
- Medication management
- Telepsychiatry services
Without accurate eligibility checks, practices risk unpaid claims and frustrated patients.
Documentation Pressure
Payers increasingly scrutinize behavioral health documentation. Therapists must balance clinically meaningful notes with compliance requirements.
A skilled mental health billing consultant often helps practices align documentation standards with payer expectations while reducing audit risks.
Why Columbus Practices Are Outsourcing Billing
Columbus has seen substantial growth in behavioral health demand over the past several years. Private practices, outpatient clinics, substance abuse treatment centers, and teletherapy providers are expanding quickly.
Growth is positive—but it also exposes weaknesses in internal billing systems.
Hiring and training in-house billing staff can become expensive and time-consuming, especially when behavioral health coding expertise is difficult to find locally. This has led many organizations toward outsourced mental health billing solutions.
The Financial Reality of In-House Billing
Maintaining an internal billing department often includes:
- Salaries and benefits
- Software expenses
- Staff training
- Compliance management
- Coding updates
- Denial management
- Credentialing administration
For smaller and mid-sized practices, those operational costs can outweigh the benefits of keeping billing internal.
Mental health medical billing services outsourcing allows providers to access specialized expertise without carrying the full overhead burden.
What Specialized Mental Health Billing Actually Improves
Some providers assume outsourcing only means someone submits claims on their behalf. In reality, experienced behavioral health billing teams manage much more than claim entry.
A high-performing mental health billing agency typically works across the entire revenue cycle.
Accurate Coding Support
Behavioral health coding changes regularly, especially with telehealth regulations and payer updates. Specialized billers understand:
- Psychotherapy CPT codes
- Add-on codes
- Crisis intervention billing
- Evaluation and management coding
- Behavioral assessment billing
- Substance abuse treatment coding
Correct coding directly impacts reimbursement speed and compliance.
Faster Claims Processing
Efficient billing systems reduce delays between service delivery and reimbursement. Instead of claims sitting in queues for days, they are reviewed and submitted quickly.
That acceleration improves cash flow consistency for practices.
Denial Prevention Strategies
Strong billing teams focus on prevention rather than reactive correction.
A proactive mental health billing and coding company may:
- Review claims before submission
- Verify authorizations
- Audit documentation
- Identify recurring denial patterns
- Monitor payer policy changes
Reducing denials saves substantial administrative time.
Real-World Example: A Growing Therapy Practice in Columbus
Imagine a mid-sized therapy clinic with six therapists and one psychiatric nurse practitioner.
Initially, the practice managed billing internally using a front-desk coordinator. As patient volume increased, billing errors became more frequent. Denials started rising, especially for telehealth claims. Accounts receivable aged beyond 90 days, and staff spent hours calling insurance companies instead of helping patients.
The clinic eventually partnered with a behavioral health-focused billing provider.
Within several months:
- Claim turnaround improved
- Denials decreased
- Outstanding AR dropped
- Providers spent less time on administrative tasks
- Revenue became more predictable
This type of outcome is one reason outsourced mental health billing continues gaining momentum among behavioral health providers.
Choosing the Right Mental Health Billing Partner
Not every billing provider understands behavioral healthcare. Some companies handle multiple specialties but lack deep knowledge of mental health reimbursement nuances.
When evaluating mental health billing companies, providers should look beyond pricing alone.
Experience in Behavioral Health Matters
A company experienced in orthopedic or cardiology billing may still struggle with psychotherapy workflows.
Behavioral health practices should ask:
- Do they specialize in mental health?
- Are they familiar with local and national payer trends?
- Can they manage telehealth billing accurately?
- Do they understand behavioral health documentation standards?
The answers often determine long-term billing success.
Transparency Is Essential
Practices should have clear visibility into:
- Claims status
- Denial trends
- Revenue reports
- Aging AR
- Payment timelines
Reliable billing partners provide consistent reporting and communication instead of operating behind the scenes without accountability.
Credentialing Support Is Often Overlooked
Credentialing delays are a major reason providers lose revenue. If a therapist or psychiatrist is not properly credentialed with insurers, claims may be rejected entirely.
Many providers prefer billing services for mental health providers that also assist with credentialing management because it creates a more coordinated workflow.
The Rise of Telehealth Has Changed Behavioral Health Billing
Telehealth transformed mental healthcare delivery, but it also introduced new billing complexities.
Behavioral health practices must now manage:
- State-specific telehealth rules
- Modifier requirements
- Audio-only billing regulations
- Cross-state licensing considerations
- Evolving payer policies
Practices relying on outdated billing systems often struggle to keep up.
A top outsource mental health billing company continuously monitors payer updates so providers don’t have to track every regulatory change themselves.
Small Errors That Cost Practices Thousands
Mental health practices sometimes underestimate how costly minor billing issues can become over time.
For example:
- Repeated undercoding reduces long-term revenue
- Missing authorizations create preventable denials
- Delayed claim submissions lead to missed filing deadlines
- Poor follow-up increases unpaid balances
Even a small denial percentage can translate into significant annual revenue loss.
This is why many providers view outsourced billing not as an expense, but as a financial protection strategy.
Beyond Billing: Improving the Entire Patient Experience
Revenue cycle efficiency affects more than finances.
When administrative systems function smoothly:
- Patients receive clearer billing information
- Front-desk staff spend less time resolving insurance issues
- Providers focus more on treatment
- Scheduling becomes more efficient
- Practice operations feel less stressful overall
Financial stability also allows clinics to invest in growth, staffing, and patient care improvements.
An experienced mental health billing consultant often helps practices identify operational inefficiencies beyond billing itself.
Compliance Risks Continue to Grow
Behavioral healthcare providers face increasing scrutiny from insurers and regulatory bodies. Documentation audits, payer reviews, and coding compliance checks are becoming more common.
Working with the best outsource mental health billing and coding company can help practices reduce exposure to:
- Incorrect coding
- Incomplete documentation
- Billing inconsistencies
- Regulatory violations
- Reimbursement disputes
Strong compliance support is particularly important for multi-provider practices and organizations expanding into telehealth services.
Why Generic Billing Models Often Fail in Behavioral Health
Behavioral health reimbursement requires more specialized attention than many general billing vendors provide.
A generalist billing service may not fully understand:
- Time-based psychotherapy coding
- Behavioral health authorization rules
- Substance abuse treatment billing
- Coordination of benefits in therapy settings
- Mental health-specific payer edits
That lack of specialization can quietly reduce collections over time.
Practices increasingly prefer a dedicated mental health billing agency that understands the operational realities of therapy and psychiatric care.
Frequently Asked Questions
What makes mental health billing different from general medical billing?
Mental health billing often involves time-based CPT coding, authorization requirements, telehealth regulations, and stricter documentation standards. Behavioral health claims also face higher denial rates if coding or payer rules are not followed correctly.
Why are mental health claim denials so common?
Common reasons include incorrect modifiers, missing authorizations, documentation inconsistencies, credentialing issues, and payer-specific behavioral health policies. Even small errors can result in delayed or denied reimbursements.
Is outsourced mental health billing cost-effective for small practices?
In many cases, yes. Smaller practices may struggle with staffing, training, software costs, and payer follow-up internally. Outsourcing can reduce overhead while improving reimbursement accuracy and collections.
How do mental health billing companies improve cash flow?
Specialized billing providers reduce claim errors, speed up submission timelines, manage denials proactively, and improve insurance follow-up processes. Faster reimbursements help stabilize revenue cycles.
What should providers look for in a mental health billing company?
Providers should evaluate behavioral health expertise, transparency, reporting systems, denial management processes, telehealth knowledge, and credentialing support before choosing a billing partner.
Can a billing company help with telehealth reimbursement?
Yes. Experienced behavioral health billing providers stay updated on telehealth coding rules, payer policies, modifiers, and compliance requirements to ensure accurate claim submission.
Final Thoughts
Mental healthcare providers in Columbus are navigating an increasingly demanding administrative environment. Insurance complexities, changing payer policies, telehealth expansion, and rising compliance expectations have made billing far more challenging than it was just a few years ago.
Practices that rely on outdated workflows or non-specialized billing support often experience avoidable denials, delayed reimbursements, and operational strain. In contrast, providers that invest in specialized behavioral health billing expertise are typically better positioned for financial stability and long-term growth.
Strong billing support is no longer just about submitting claims. It now includes accurate coding oversight, denial prevention, credentialing coordination, payer communication, and broader revenue cycle management strategies that protect the financial health of a practice.
For organizations seeking dependable support, companies like 247 Medical Billing Services provide integrated solutions that combine medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services tailored to modern healthcare operations. For behavioral health practices especially, working with experienced specialists can help reduce administrative burdens while allowing providers to stay focused on patient care.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Jocuri
- Gardening
- Health
- Home
- Literature
- Music
- Networking
- Alte
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness


