-
Fil d’actualités
- EXPLORER
-
Pages
-
Groupes
-
Evènements
-
Reels
-
Blogs
-
Offres
-
Emplois
Mental Health Billing and Credentialing Services in USA: Complete Guide for Providers
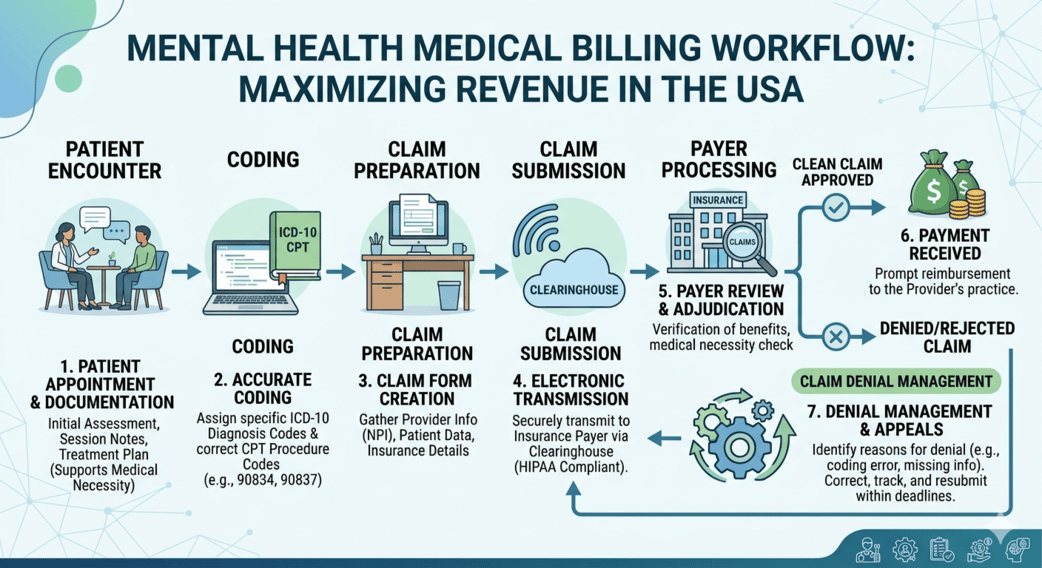
Mental health practices across the USA face a unique combination of administrative, regulatory, and financial challenges. From complex payer rules to credentialing delays, managing the revenue cycle efficiently requires both expertise and consistency. This is where mental health billing and credentialing services play a critical role.
A well-structured billing system not only improves cash flow but also reduces claim denials, ensures compliance, and allows providers to focus on patient care. Whether you are an independent therapist, a group practice, or a behavioral health clinic, understanding how billing and credentialing work together is essential for long-term success.
Why Mental Health Billing Requires Specialized Expertise
Mental health billing differs significantly from general medical billing. It involves therapy sessions, psychiatric evaluations, medication management, and long-term care plans—all of which come with specific coding and documentation requirements.
Key challenges include:
- Frequent claim denials due to incorrect coding and documentation
- Complex insurance policies for behavioral health treatments
- Time-consuming prior authorizations and eligibility verification
- Constant updates in payer guidelines and compliance regulations
Because of these complexities, many providers seek professional mental health billing solutions to streamline operations and improve reimbursement rates.
Understanding Mental Health Billing and Credentialing Services
Mental health billing and credentialing services cover two critical components of practice management:
Billing Services:
These involve the entire revenue cycle—from patient registration to claim submission, payment posting, and denial management. Efficient billing for mental health providers ensures accurate claim processing and timely reimbursements.
Credentialing Services:
Credentialing is the process of enrolling providers with insurance networks. Without proper credentialing, providers cannot bill insurance companies, making it a foundational step in billing for mental health services.
Together, these services ensure that providers are authorized, compliant, and financially stable.
Core Components of Mental Health Billing
A strong mental health billing process includes several interconnected steps:
1. Patient Eligibility Verification
Before providing services, verifying insurance coverage ensures that billing for mental health services is accurate and reduces claim rejections.
2. Accurate Coding
Coding and billing for mental health services rely on CPT and ICD codes specific to therapy sessions, psychiatric services, and behavioral treatments. Errors in coding can lead to delays or denials.
3. Claim Submission
Timely and accurate claim submission is essential for faster reimbursements in medical billing for mental health.
4. Payment Posting and Reconciliation
Tracking payments ensures transparency and helps identify underpayments or discrepancies.
5. Denial Management and Appeals
Efficient follow-up and appeals improve revenue recovery and reduce financial losses.
The Importance of Credentialing in Mental Health Practices
Credentialing is often overlooked but is critical to revenue generation. Without proper enrollment, even correctly submitted claims will be denied.
Key aspects include:
- Insurance panel enrollment
- Re-credentialing and updates
- Compliance with payer requirements
- Managing provider documentation
Professional mental health billing and credentialing services help avoid delays and ensure providers are always in-network with major insurers.
Benefits of Outsourcing Mental Health Billing
Many practices are now opting for outsourcing mental health billing due to the increasing complexity of administrative tasks.
1. Improved Revenue Cycle Efficiency
Outsourced billing for mental health ensures claims are processed faster and more accurately.
2. Reduced Administrative Burden
Providers can focus on patient care instead of handling paperwork and follow-ups.
3. Expertise and Compliance
Experienced teams stay updated with changing regulations and payer requirements.
4. Cost-Effective Operations
Working with a cheap outsource mental health billing company can reduce overhead costs while maintaining quality.
5. Advanced Technology and Reporting
Modern mental health billing solutions include analytics, reporting, and performance tracking.
Who Needs Mental Health Billing Services?
Billing services for mental health are beneficial for:
- Independent therapists and counselors
- Psychiatrists and psychologists
- Behavioral health clinics
- Substance abuse treatment centers
- Telehealth mental health providers
Whether small or large, every practice can benefit from structured mental health medical billing systems.
Medicare and Insurance Billing Considerations
Billing Medicare for mental health services requires strict adherence to documentation and coding guidelines. Common challenges include:
- Session time limitations
- Specific CPT code requirements
- Documentation for medical necessity
- Compliance with telehealth policies
Professional billing services for mental health clinics ensure that all claims meet Medicare standards, reducing rejection rates.
Key Features of the Best Mental Health Billing Services
Choosing the best outsource mental health billing and coding services involves evaluating several factors:
- Industry-specific expertise in behavioral and mental health billing services
- Transparent pricing and reporting
- Dedicated account management
- Strong denial management processes
- HIPAA-compliant systems
A reliable partner can significantly improve the financial health of your practice.
Common Mistakes in Mental Health Billing
Avoiding common errors is essential for maintaining a smooth revenue cycle:
- Incorrect or outdated coding
- Missing documentation
- Failure to verify patient eligibility
- Delayed claim submission
- Ignoring denied claims
By implementing structured mental health billing processes, practices can minimize these risks.
How Technology is Transforming Mental Health Billing
Digital tools and automation are reshaping billing for mental health therapists and clinics. Modern systems offer:
- Automated claim submission
- Real-time eligibility checks
- AI-driven denial prediction
- Integrated EHR and billing platforms
These innovations enhance efficiency and accuracy in billing mental health services.
Why Choose Professional Mental Health Billing Services
Managing billing internally can be overwhelming, especially with growing patient volumes and regulatory changes. Partnering with experts in medical billing for mental health ensures:
- Higher claim acceptance rates
- Faster reimbursements
- Reduced administrative workload
- Better financial insights
Outsourced billing for mental health provides scalability and consistency that in-house teams often struggle to maintain.
Conclusion
Mental health billing and credentialing services are essential for ensuring financial stability and operational efficiency in today’s healthcare environment. From accurate coding and timely claim submission to proper credentialing and compliance, every step plays a vital role in revenue cycle success.
By adopting professional mental health billing solutions or choosing outsourcing mental health billing, providers can focus on delivering quality care while maintaining a steady revenue flow. For practices looking to grow sustainably, investing in expert billing services for mental health is no longer optional—it is a strategic necessity.
Organizations like 247 Medical Billing Services support providers with comprehensive medical billing services, medical coding services, medical billing and coding services, revenue cycle management services, and credentialing services, helping mental health practices achieve efficiency, compliance, and consistent growth.
FAQs
1. What are mental health billing and credentialing services?
They include managing the entire billing process and enrolling providers with insurance companies to ensure claims are accepted and reimbursed.
2. Why is credentialing important for mental health providers?
Credentialing allows providers to bill insurance companies. Without it, claims will be denied regardless of accuracy.
3. Is outsourcing mental health billing a good option?
Yes, outsourcing mental health billing improves efficiency, reduces errors, and ensures compliance with payer guidelines.
4. What services are included in mental health billing solutions?
They typically include eligibility verification, coding, claim submission, denial management, and reporting.
5. How does Medicare billing differ for mental health services?
Billing Medicare for mental health services requires strict documentation, specific CPT codes, and adherence to federal guidelines.
6. Who can benefit from billing services for mental health clinics?
Therapists, psychiatrists, group practices, and behavioral health centers can all benefit from professional billing services.
7. How do I choose the best outsource mental health billing and coding services?
Look for experience, transparency, compliance, technology, and strong client support when selecting a billing partner.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Jeux
- Gardening
- Health
- Domicile
- Literature
- Music
- Networking
- Autre
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness


